Introduction
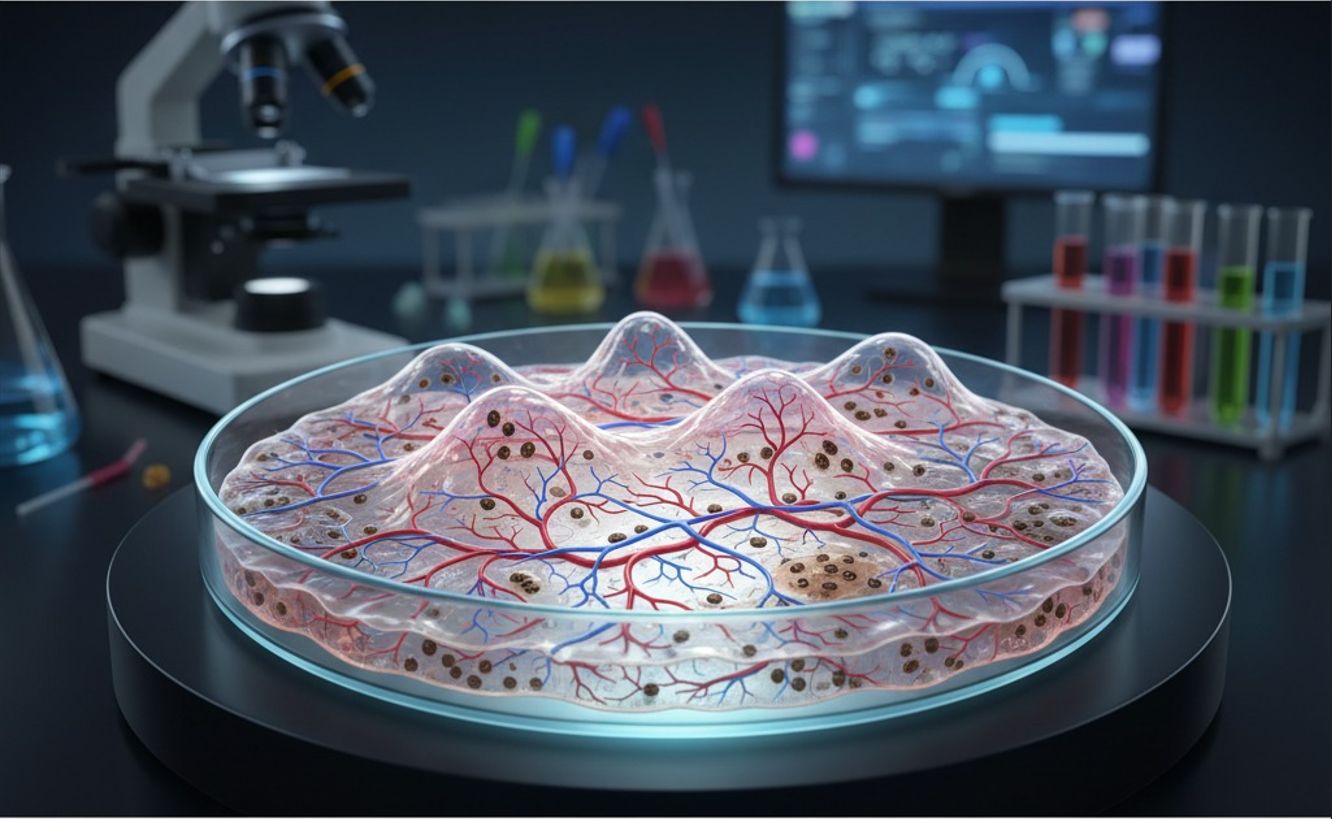
Lab-grown human skin: University of Queensland researchers created a fully functioning human skin model with vessels, pigmentation and appendages that could change grafts and dermatology care.
Quick definition
A 3D skin organoid grown from reprogrammed human stem cells that includes blood vessels, hair follicles, pigmentation and immune cells.
Context
Scientists at UQ's Frazer Institute spent six years developing a skin organoid from human cells converted into stem cells. The model reproduces key structures—capillaries, multiple tissue layers and immune components—making it one of the most life-like lab skins globally.
Lab-grown human skin: the challenge addressed
Dermatology research relied on simplified models; grafts and wound treatments faced limited effectiveness and infection risk. A realistic model reduces experimental uncertainty and accelerates drug and therapy development.
Solution and practical impact
The team engineered microvessels into the organoid, producing tissue that develops like natural skin with pigmentation, follicles, nerves and its own blood supply. Immediate uses include better grafts, studies on psoriasis, atopic dermatitis, scleroderma, genetic conditions, and progress in regenerative medicine and precision dermatology.
"This is the most life-like skin model that's been developed anywhere in the world and will allow us to study diseases and test treatments more accurately."
Dr Abbas Shafiee
"This skin model will enable us to further progress those treatments, along with wound healing, regenerative medicine and precision dermatology."
Professor Kiarash Khosrotehrani
Conclusion
UQ's lab-grown human skin offers a major step forward for grafts and dermatology; vascularization and pigmentation enable more accurate testing, though clinical translation will require extensive validation.
FAQ
What is lab-grown human skin?
It is a 3D skin organoid created from reprogrammed human stem cells that mimics structural and functional aspects of human skin, including vessels and pigmentation.
How can lab-grown human skin improve grafts?
By providing tissue with microcirculation and realistic architecture, it can improve integration, lower infection risk and increase graft effectiveness.
Which skin conditions could benefit from this model?
Psoriasis, atopic dermatitis, scleroderma and some genetic skin disorders can be studied more accurately using this model.
When might clinical applications become available?
Extensive preclinical and clinical studies are still needed; the discovery is promising but clinical translation will take time and safety validation.